 Athlete's foot is a common fungal infection that affects the skin on the feet, particularly between the toes. It's a condition that can cause discomfort and inconvenience, but with proper
Read more
Athlete's foot is a common fungal infection that affects the skin on the feet, particularly between the toes. It's a condition that can cause discomfort and inconvenience, but with proper
Read more
-
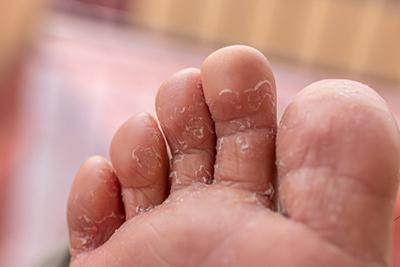
Athlete's Foot: Recognizing and Treating Fungal Infections
posted: May 01, 2024.
 Athlete's foot is a common fungal infection that affects the skin on the feet, particularly between the toes. It's a condition that can cause discomfort and inconvenience, but with proper
Read more
Athlete's foot is a common fungal infection that affects the skin on the feet, particularly between the toes. It's a condition that can cause discomfort and inconvenience, but with proper
Read more
-
Diabetic Foot Care: Importance, Tips, and Warning Signs
posted: Apr. 08, 2024.
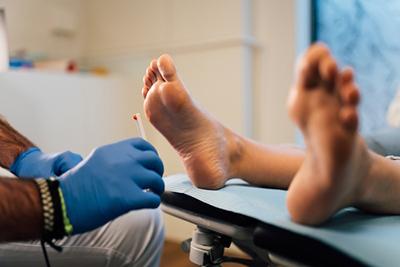 When you’re dealing with diabetes, you may understand that one of the most important things you can do is care for your feet. For individuals living with diabetes, proper foot
Read more
When you’re dealing with diabetes, you may understand that one of the most important things you can do is care for your feet. For individuals living with diabetes, proper foot
Read more
-
Symptoms of an Ingrown Toenail
posted: Apr. 01, 2024.
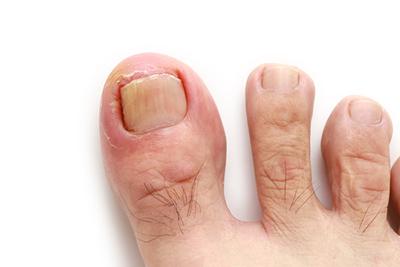 Ingrown toenails are painful and ugly. They can make it difficult to put on shoes, to stand, and to walk without pain. An ingrown toenail can decrease your mobility. Your
Read more
Ingrown toenails are painful and ugly. They can make it difficult to put on shoes, to stand, and to walk without pain. An ingrown toenail can decrease your mobility. Your
Read more
-
Treating Plantar Fasciitis
posted: Mar. 15, 2024.
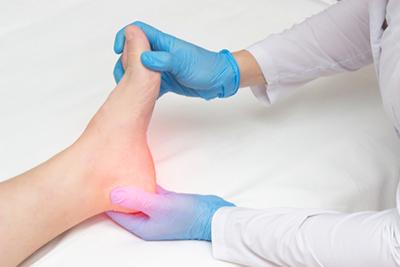 If you are experiencing stabbing, aching heel pain on the side of your foot, or running across your heel, you could have a very common condition known as plantar fasciitis.
Read more
If you are experiencing stabbing, aching heel pain on the side of your foot, or running across your heel, you could have a very common condition known as plantar fasciitis.
Read more
-
Managing Your Heel Pain
posted: Mar. 01, 2024.
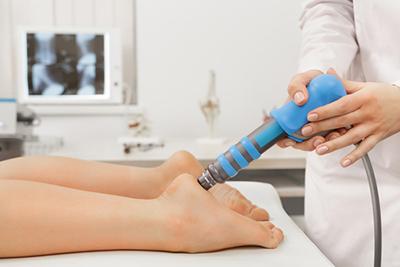 Your heels are nature’s shock absorbers, providing a cushion for standing, walking, and running. If you’ve ever experienced heel pain, you already know how it can impact your life. The
Read more
Your heels are nature’s shock absorbers, providing a cushion for standing, walking, and running. If you’ve ever experienced heel pain, you already know how it can impact your life. The
Read more
-
The Role of Podiatry in Managing Foot and Ankle Fractures
posted: Feb. 12, 2024.
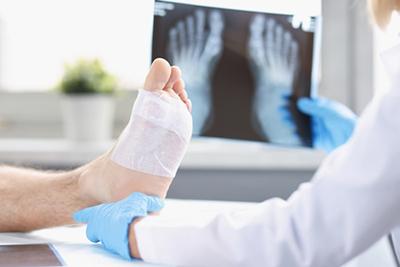 Foot and ankle fractures are a common problem, especially as you get older. Bones become more brittle, and you are less flexible than you once were. Foot and ankle fractures
Read more
Foot and ankle fractures are a common problem, especially as you get older. Bones become more brittle, and you are less flexible than you once were. Foot and ankle fractures
Read more
-
What You Need To Know About Ingrown Toenails
posted: Feb. 01, 2024.
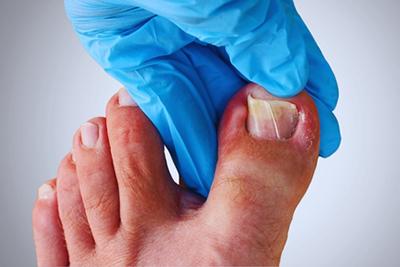 Ingrown toenails can happen to anyone. If you have an ingrown toenail, chances are it’s difficult to put on shoes and want to walk around. Your podiatrist can help with
Read more
Ingrown toenails can happen to anyone. If you have an ingrown toenail, chances are it’s difficult to put on shoes and want to walk around. Your podiatrist can help with
Read more
-
Sports Podiatry: Addressing Foot and Ankle Injuries in Athletes
posted: Jan. 08, 2024.
 As an athlete, you know how critical it is to stay at the top of your game and remain in optimal physical shape. Your feet and ankles are the foundation
Read more
As an athlete, you know how critical it is to stay at the top of your game and remain in optimal physical shape. Your feet and ankles are the foundation
Read more
-
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
posted: Jan. 01, 2024.
 Do you have foot problems? Do your feet hurt all the time? If so, you need to discover the benefits of orthotics. This common treatment, available from your podiatrist, can
Read more
Do you have foot problems? Do your feet hurt all the time? If so, you need to discover the benefits of orthotics. This common treatment, available from your podiatrist, can
Read more
-
Diabetic Foot Care: Preventing Complications and Maintaining Foot Health
posted: Dec. 07, 2023.
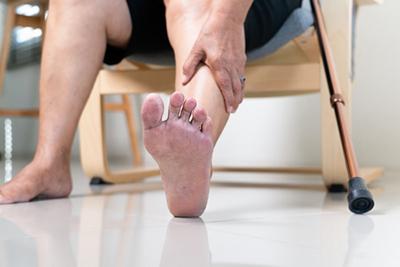 Diabetes, a condition affecting how your body uses sugar, impacts various organs, including your feet. High blood sugar can lead to nerve damage (neuropathy) and poor circulation, increasing the risk
Read more
Diabetes, a condition affecting how your body uses sugar, impacts various organs, including your feet. High blood sugar can lead to nerve damage (neuropathy) and poor circulation, increasing the risk
Read more
-
Preventing Foot Injuries: Tips for Proper Foot Care and Injury Avoidance
posted: Dec. 01, 2023.
 If you experience a foot injury, it can dramatically impact your quality of life. Depending on the injury, foot injuries can lead to loss of mobility, inability to drive, lost
Read more
If you experience a foot injury, it can dramatically impact your quality of life. Depending on the injury, foot injuries can lead to loss of mobility, inability to drive, lost
Read more
-
The Benefits of Seeing a Podiatrist
posted: Nov. 07, 2023.
 A podiatrist is a specialized medical professional devoted to the diagnosis, treatment, and care of conditions related to the feet, ankles, and lower extremities. Their expertise encompasses many issues, from
Read more
A podiatrist is a specialized medical professional devoted to the diagnosis, treatment, and care of conditions related to the feet, ankles, and lower extremities. Their expertise encompasses many issues, from
Read more
-
The Benefits Of Orthotics
posted: Nov. 01, 2023.
 Orthotics are custom-made shoe inserts or insoles designed to support and correct irregularities in foot function. They aim to alleviate various foot and ankle conditions, providing relief and improved mobility.
Read more
Orthotics are custom-made shoe inserts or insoles designed to support and correct irregularities in foot function. They aim to alleviate various foot and ankle conditions, providing relief and improved mobility.
Read more
-
When To See a Podiatrist
posted: Oct. 06, 2023.
 A podiatrist is an expert at diagnosis and treatment of foot, ankle, and toe conditions. A podiatrist can help you enjoy healthy feet, so you can stay active. Visiting your
Read more
A podiatrist is an expert at diagnosis and treatment of foot, ankle, and toe conditions. A podiatrist can help you enjoy healthy feet, so you can stay active. Visiting your
Read more
-
The Importance of Diabetic Care
posted: Oct. 01, 2023.
 When you’re dealing with diabetes, it’s important that you’re getting all the care that you need to ensure every part of your body. One big issue is making sure that
Read more
When you’re dealing with diabetes, it’s important that you’re getting all the care that you need to ensure every part of your body. One big issue is making sure that
Read more
-
Treating Your Bunion Symptoms
posted: Sep. 15, 2023.
 Bunions are a common problem. In fact, over half of the women in the United States have developed a bunion at some point, according to the American Academy of Orthopedic
Read more
Bunions are a common problem. In fact, over half of the women in the United States have developed a bunion at some point, according to the American Academy of Orthopedic
Read more
Contact Us
Our Location
Find us on the map
Hours of Operation
Our Regular Schedule
Monday:
9:00 AM-5:00 pm
Tuesday:
9:00 am-5:00 pm
Wednesday:
9:00 am-5:00 pm
Thursday:
9:00 am-5:00 pm
Friday:
9:00 am-5:00 pm
Saturday:
Closed
Sunday:
Closed